Paramedic practice around the world is rapidly evolving (Vertesi, 1978; Munger, 2000; O'Meara et al, 2012; Batt, 2016), demonstrated by the international transition towards third-level education (Donaghy, 2008; Hou et al, 2013; Maguire et al, 2016; Caffrey et al, 2019).
In Ireland, healthcare has been moving towards a collaborative, integrated system (Darker, 2013), exemplified by the management of cardiovascular emergencies, which requires cooperation between prehospital emergency medical services (EMS), emergency departments, cardiology services and primary percutaneous coronary intervention (PPCI) centres (Tubaro et al, 2011; Bagai et al, 2014; Jennings et al, 2017).
Accurate and timely ECG interpretation can reduce time to reperfusion therapy, lowering morbidity and mortality, and reducing ‘false-positive activations’ of PPCI centres (Le May et al, 2010; Nam et al, 2014; Quinn et al, 2014; Squire et al, 2014; Jennings et al, 2017). Furthermore, clinically significant abnormalities on a prehospital ECG may resolve before assessment in the emergency department (Davis et al, 2014). Consequently, the successful care pathway for a patient with acute coronary symptoms often hinges on the EMS interpretation of 12-lead ECGs (Cheskes et al, 2011).
The role of EMS practitioners has evolved from a traditional ambulance driver to the modern paramedic (Williams et al, 2012). In Ireland, advanced paramedics are paramedics with additional training that allows them to perform advanced life support skills and interventions (Cummins et al, 2013; Knox et al, 2014).
The benefits of proficient recognition of ST elevation by EMS practitioners are well established (Millar-Craig et al, 1997; May et al, 2006; Cantor et al, 2012; Funder et al, 2020). However, shortcomings in paramedics' ECG interpretation have also been identified, potentially resulting in missed or inappropriate PPCI centre activation (Mencl et al, 2013).
Additionally, while a patient with an ST-elevation myocardial infarction (STEMI) or a new left bundle branch block in Ireland can be brought directly to a PPCI centre if it is within a 90-minute drive (O'Donnell, 2012), the ESC guidelines indicate that other ECG changes, ‘in the absence of characteristic ST elevation’, can indicate acute coronary occlusion, and might require emergency reperfusion therapy (Ibanez et al, 2018). Therefore, improving paramedics' interpretation of ECGs could result in better patient outcomes.
The aim of this study is to investigate the National Ambulance Service of Ireland (NAS) view of paramedics and advanced paramedics on ways to improve their ECG interpretation abilities.
Methods
A mixed-methods study combining quantitative and qualitative analysis was designed (Schifferdecker and Reed, 2009). The authors used the explanatory model (Schifferdecker and Reed, 2009), with the quantitative aspect performed initially, and informing the qualitative aspect.
The study received ethical approval from the University of Limerick Faculty of Education and Health Sciences research ethics committee (ethical approval reference 2019_12_29_EHS).
Participants and setting
The NAS employs more than 1600 individuals divided between three operational regions: NAS East; NAS West; and NAS South. The NAS research committee, being aware of the demands on paramedics, wanted to limit research fatigue. Therefore, the study was restricted to the Dublin and North Leinster hubs. This area in the NAS East region employs more than 400 paramedics and advanced paramedics and includes 21 ambulance stations (NAS, 2015) (Figure 1).
Quantitative arm
Recruitment
Invitations to participate in the study were disseminated via multiple channels: email by the local training and development officers; social media activity; and posters displayed in the targeted ambulance stations. Interested paramedics and advanced paramedics were emailed a comprehensive study information sheet, including a consent form and a link to the initial survey. Participation was incentivised by an offer of entry to a draw for a modest gift card.
Data collection
The quantitative data collection instrument consisted of an anonymous, web-based questionnaire powered by Qualtrics. After confirming informed consent, the following demographic details were sought: number of years in the NAS; clinical level; and number of years qualified.
The survey assessed the perceived diagnostic utility of listed ECG interpretation criteria, the preferred time and device to access electronic educational content, and suggestions on ways to improve confidence in ECG interpretation. The survey concluded with a contact form if participants wanted to volunteer to be interviewed.
Data analysis
The data were checked in the first instance by a gatekeeper employed by the academic institution to ensure anonymity. The database generated from the survey was imported into IBM SPSS (v. 26) software to compute descriptive statistics including frequencies, means, standard deviations and one sample t-test.
Qualitative arm
A research protocol was developed, based on the COREQ guidelines—the consolidated criteria for reporting qualitative research (Tong et al, 2007).
Recruitment
A random sequence generator (Haahr, 2009) was used to select volunteers to interview from the contact forms submitted. A number of volunteers were excluded for having recently worked with the primary researcher. Informed consent was sought at the start of each interview. Interviews were conducted until data saturation was reached and no further themes emerged. While there is no standardised minimum number of interviews required for qualitative research, Smith and Shinebourne (2012) proposed a minimum of three. In this study, 11 mobile-phone interviews were conducted.
Data collection
An interview guide was developed initially by the primary researcher, using data gathered from the quantitative arm, and refined by suggestions from the other members of the team. The interview guide was used for the first six interviews, then modified in the light of emerging themes. The last five interviews used the final interview guide.
The interviews were digitally recorded and transcribed verbatim by the primary researcher. A small number of field notes were also taken by the primary researcher during the interview process.
Data analysis
Initially, each transcript was read and re-read by all three researchers. Two interviews were randomly selected, manually and independently coded by two of the researchers, then checked for consistency by the third one.
A list of codes was created and used by the primary researcher to guide the coding of the remaining interviews, and the list was amended as required. The entire process of amending the code list was checked for consistency by the other researchers. The resulting qualitative data were interpreted using the template analysis approach described by Brooks et al (2015).
Data saturation
Interviews were carried out, transcribed and coded until they stopped generating new themes or major new codes. Data saturation was reached at the ninth interview; another two interviews were completed to confirm saturation.
Bias mitigation
The primary researcher's role as an advanced paramedic raised the concern of interpretation bias. The research team held a number of discussions, which involved reading Reflectivity in Research Practice: an Overview of Different Perspectives (Mortari, 2015), to increase awareness and hopefully mitigate interpretation bias.
Results
Quantitative
The voluntary survey was completed by 118 prehospital practitioners, 72 paramedics and 44 advanced paramedics. Their professional experience is outlined in Table 1. Participants' mean NAS experience was 10.31 years (SD=8.42 years). The longest-serving respondent joined the NAS in 1984; the most junior joined in 2019. The longest-serving advanced paramedic joined in 2000.
| National Ambulance Service experience | Total | % |
|---|---|---|
| <5 years | 49 | 41.5 |
| 5–10 years | 25 | 21.2 |
| 10–15 years | 9 | 7.6 |
| 15–20 years | 19 | 16.1 |
| >20 years | 13 | 11.0 |
| Missing | 3 | 2.5 |
| Total | 118 | 100.0 |
| Paramedic | 72 | 61 |
| <5 years | 49 | 41.5 |
| 5–10 years | 22 | 18.6 |
| 10–15 years | 11 | 9.3 |
| 15–20 years | 12 | 10.2 |
| >20 years | 18 | 15.3 |
| Missing | 6 | 5.1 |
| Total | 118 | 100.0 |
| Advanced paramedic | 44 | 37.3 |
| <5 years | 13 | 29.5 |
| 5–10 years | 15 | 34.1 |
| 10–15 years | 12 | 27.3 |
| 15–20 years | 2 | 4.5 |
| >20 years | 1 | 2.3 |
| Missing | 1 | 2.3 |
| Total | 44 | 100.0 |
| Unspecified clinical level | ||
| Missing | 2 | 1.7 |
Figure 2 illustrates the rated usefulness of being able to recognise various ECG rhythms. A number of rhythms beyond STEMI were universally deemed useful, but more advanced ECG patterns (left ventricular hypertrophy, right ventricular strain and axis deviation) were perceived to be less so. Supraventricular tachycardia was included in the survey as an ECG pattern, although it is an umbrella term covering a number of discrete ECG findings including atrial fibrillation, atrial flutter, atrioventricular reentrant tachycardia and atrioventricular nodal reentry tachycardia. This limits interpretation of responses to that particular question.
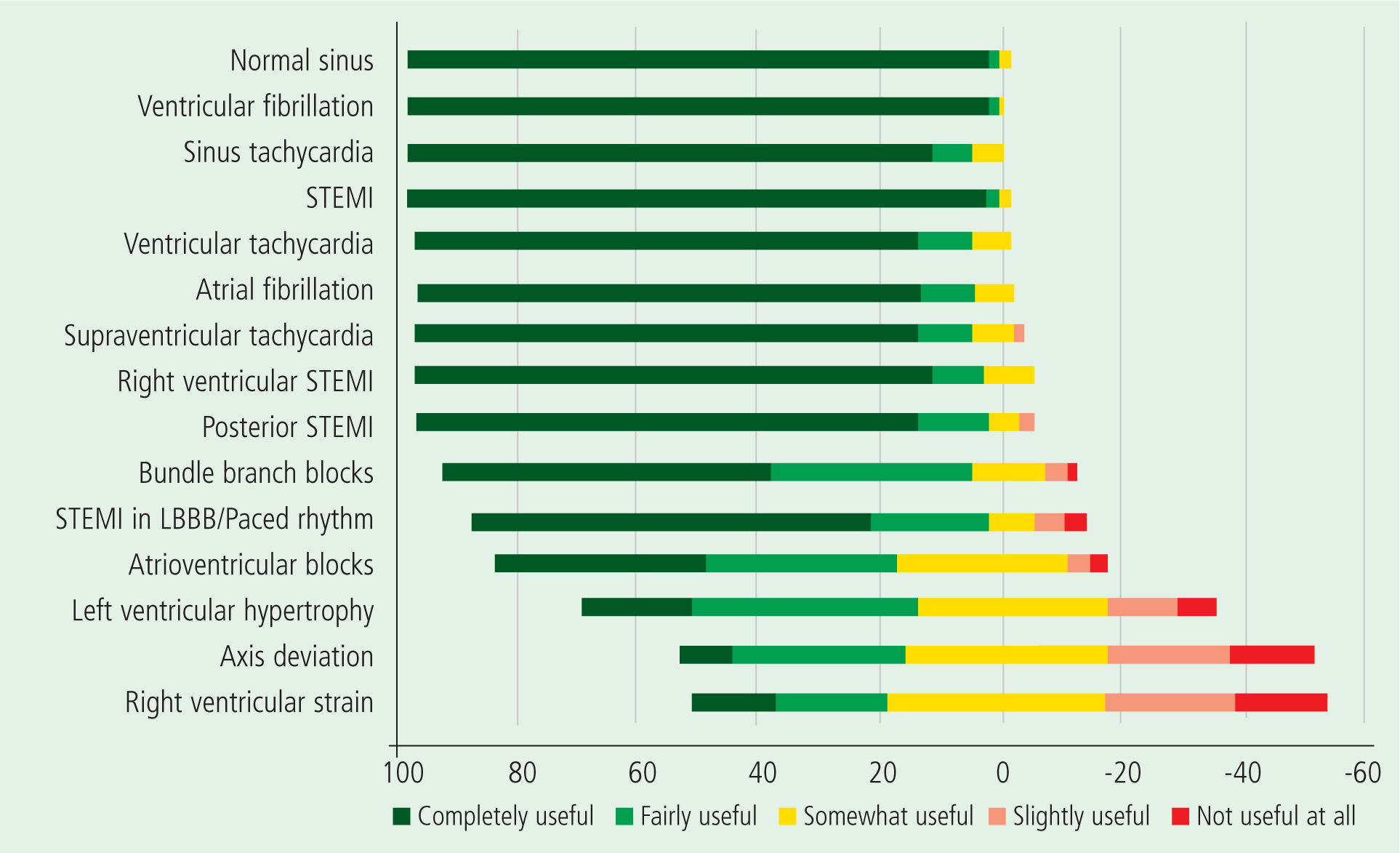
The survey concluded by asking for some suggestions to improve confidence in ECG interpretation; the resulting list then informed the qualitative interview guide. The most commonly mentioned suggestions were classroom teaching (n=60), online teaching (n=10), evaluation (n=8), online cards (n=7) and feedback (n=4).
Qualitative
Eleven participants (eight paramedics and three advanced paramedics) randomly selected out of 60 volunteers were invited to interview. On average, the interview volunteers reported a lower number of years of professional experience (mean=9; SD=7.34) than the survey respondents (mean=10.31; SD=8.42). A one sample t-test was computed and found no significant difference in mean years of experience between the overall study sample and those selected for interview.
It is the researchers' opinion that the volunteers represented the cohort adequately as they included paramedics and advanced paramedics, both experienced and newly qualified.
The template analysis of the interviews produced three main themes, which were each subdivided into subthemes (Table 3).
| Interview | Year started in the NAS | Clinical level | Paramedic qualification | AP qualification |
|---|---|---|---|---|
| 1 | 2012 | Paramedic | 2013 | |
| 2 | 2017 | Paramedic | 2019 | |
| 3 | 2005 | Paramedic | 2007 | |
| 4 | 2011 | AP | 2013 | 2018 |
| 5 | 1993 | AP | 2001 | 2006 |
| 6 | 2003 | AP | 2007 | 2011 |
| 7 | 2016 | Paramedic | 2018 | |
| 8 | 2015 | Paramedic | 2017 | |
| 9 | 2015 | Paramedic | 2018 | |
| 10 | 2018 | Paramedic | 2020 | |
| 11 | 2016 | Paramedic | 2018 |
AP: advanced paramedic; NAS: National Ambulance Service
| A profession in transition | Lifelong learning |
| Lagging professional development | Personal barriers to ECG education |
| Supporting the frontline | What resources? |
A profession in transition
Participants described how the profession is evolving and stressed the importance of lifelong learning, particularly with regard to ECG interpretation. They recognised feeling vulnerable at times because of their potential shortcomings in ECG rhythm recognition.
Lifelong learning in ECG interpretation
Both paramedics and advanced paramedics expressed a need for lifelong learning to maintain or improve ECG interpretation abilities. Participants acknowledged that learning might take place through regular clinical exposure, and also that up-to-date ECG interpretation knowledge is beneficial to paramedic practice.
Those interviewed demonstrated a will to increase their understanding of ECGs to improve their ability to deliver appropriate care to their patients:
‘It makes no difference whether you've got 20 years of experience in the ambulance service or only one, I think you're learning [about ECGs] all the time.’
‘There is a bit of an expectation on you as an advanced paramedic I think, and I'd like to have something that's kind of ongoing [regarding ECG interpretation] that's just to keep me fresh.’
Practitioner vulnerability regarding ECG interpretation
Most paramedics and advanced paramedics expressed feeling vulnerable, exposed or out of their depth at times because of their comfort level in interpreting ECGs, and that these feelings might be exacerbated by the diversity of prehospital cardiac presentations:
‘Sometimes, if you look at an ECG, literally you could be looking at a box of frogs.’
‘Afterwards, thinking about it, if I had been on my own, I would have missed that [borderline STEMI], and that kind of stressed me out.’
Conversely, one respondent reported always feeling confident about ECGs, which could be attributed to a personal attitude, to experience or to his prior role as an educator.
Lagging professional development
The interviewees identified several barriers to ECG education—some personal and others systemic. Having an awareness of these barriers may benefit the authors' recommendations for improving ECG interpretation abilities.
Personal barriers
A personal barrier is one that is specific to the individual being interviewed. Examples reported included work/life balance, lack of downtime at work, staff resistance, lack of knowledge and financial considerations.
‘If I get a chance in work, yes, we can look up stuff but you know yourself these days, getting time to get lunch is hard enough.’
Systemic barriers
A systemic barrier is defined as a shortcoming at organisational level. In the NAS, ECG interpretation is primarily taught during the paramedic and advanced paramedic training programmes. The respondents reported little emphasis on further ECG education after qualifying; 82% identified the lack of educational resources as a systemic barrier.
Other barriers included poor quality of the educational resources available, not having the scope of practice to apply extended knowledge, and difficulties because of the paucity of allocated learning time exacerbated by a heavy workload and a lagging workforce capacity:
‘I don't find that you're given any [ECG education] resources from the job. It's more so “well, we told you what we need to tell you, good luck and figure it out yourself”.’
Heterogeneous ECG interpretation skills
A direct result of the lack of educational resources provided could be the varying engagement of some respondents in self-directed learning (SDL), thus promoting heterogeneous ECG interpretation skills within prehospital practitioners at a similar clinical level.
Ten interviewees mentioned partaking in independently chosen SDL activities, ranging from traditional classroom or online education to asking colleagues or other health professionals for guidance with challenging ECGs.
Some previously identified personal barriers to ECG education can compound the diversity of SDL activities, with varying levels of financial or time commitments:
‘Looking at interesting ECGs that your colleagues have had, and then doing some courses yourself either online or in a classroom situation.’
The lack of NAS-approved resources can indirectly cause a disparity in levels of education and knowledge between practitioners at similar grades.
Another drawback of not having officially recognised ECG learning material might be the absence of a scope of practice to apply additional knowledge, potentially discouraging practitioners from undertaking further education in the first instance.
Supporting the frontline
Interviewees identified several ECG educational resources they would like to be given access to.
Type of resources
All the respondents expressed the need for consistent, further ECG educative material across the NAS.
Additional training could take place in a traditional environment or online. It could also be classified by its temporal relation to the patient encounter. Some training could take place outside of patient care, and generate knowledge that could used later during a patient assessment. The learning-before-action interventions suggested were universally seen as beneficial and included classroom or online teaching. There was no consensus as to whether these needed to be concluded with an assessment of competencies.
There was no consensus regarding in-action training resources, but the availability of a field guide was generally seen as potentially beneficial.
Post-action resources were reported as already widely used within the NAS, primarily through an informal feedback network with the help of colleagues or other health professionals. There is, however, an awareness that the feedback might not be consistent, and could benefit from becoming an official process.
There was little consensus on any of the other resources on the list generated by the survey, such as books, online books, online cards and placements:
‘[Regarding ECGs], I think we need to do a little bit of classroom stuff as part of our annual or even two-yearly sorts of updates.’
‘I do think that [ECG feedback from the emergency department would] be very good, because I found that the people who were giving the feedback were very open to questions and stuff. I think it would be a very good service or asset if it were possible to have.’
Type of device
There was also no consensus on what device would be best for accessing electronic content. Mobile phones were seen by some as a practical way to access information regardless of location, but some felt they were inappropriate devices to use during patient care.
The electronic patient care report (ePCR), a software package used across Ireland to document prehospital care, is seen by some as the perfect device to access educative material. However, others reported finding the ePCR too complicated as it is, and found practitioners could potentially become engrossed in the tablet to the detriment of patient care:
‘I think it gives a very bad impression to the patient if you're looking at your phone.’
Discussion
The interviews demonstrated an appetite for further ECG education, and a sense of vulnerability regarding ECG interpretation, among both paramedics and advanced paramedics in the cohort examined.
Interviewees were in favour of more traditional classroom training, more access to online activities, access to an official feedback mechanism to document the interpretation of complex ECGs, and the addition of a field guide to the cardiac monitoring equipment.
Paramedic practice, in Ireland and around the world, has evolved significantly over the past 20 years (Batt and Buick, 2015). This evolution has created many challenges for the education of paramedics (Smith, 2017). An adult learning theory described by Knowles (1968) characterises the mature adult learner as a self-directed being with an essential thirst for applicable knowledge. In this context, it is perhaps natural that more than 90% of practitioners interviewed mentioned taking part in SDL.
SDL has been shown to be an effective learning method for the continuous education of practising medical professionals (Mamary and Charles, 2003), particularly so for the rural physician (Curran et al, 2016), whose remote practice might be compared to the prehospital environment.
During interviews, it became clear that the lack of official ECG educational resources is resulting in heterogeneous SDL activity and varying levels of competence in ECG interpretation among practitioners at similar clinical levels.
Group-orchestrated self-directed learning (GOSDL) is an umbrella term proposed by the authors to describe a process of further education, making use of the resources identified by a cohort of practitioners (group-orchestrated) at a time that suits the individual (self-directed). By providing the training resources, the NAS could ensure consistency of care throughout the organisation, and promote expansion of scope of practice.
The pre-action learning activities identified during the study—traditional classroom and online learning—have previously been compared. A study by McCutcheon et al (2015) found that ‘online learning for teaching clinical skills is no less effective than traditional means’. In addition, the propensity to use a web-based learning programme has been shown to be independent of reported learning styles (Nilsson et al, 2012). The establishment of a blended ECG learning programme in the NAS, including a combination of traditional lectures and online teaching, may provide a comprehensive ECG learning environment, affording the practitioner the opportunity for both directed and self-directed learning.
Considering in-action learning methods, Hale et al (2011) assessed a flip book of illustrated ECG tracings and their associated diagnostic criteria, which was placed in ambulances. The authors concluded that a flip book without any additional support was not effective for improving competence in 12-lead ECG interpretation. While such a field guide was identified as potentially beneficial by respondents, the onus might be on the NAS to provide it as part of a comprehensive ECG training package.
The post-action learning opportunity of feedback is well documented in Improving Use of Prehospital 12-Lead Electrocardiography for Early Identification and Treatment of Acute Coronary Syndrome and ST-Elevation Myocardial Infarction (Daudelin et al, 2010). An official feedback mechanism to improve the interpretation of challenging ECGs is regarded by most respondents as a genuine opportunity for learning.
Work/life balance was a concern to most practitioners. In Ireland, the prehospital care regulator declared a requirement of 2 weeks of continuing professional development (CPD) annually for paramedics and advanced paramedics (Pre-Hospital Emergency Care Council, 2008). Consequently, the authors assessed training resources and their impact on the practitioners' time off. Traditional classroom sessions may have been favoured by practitioners as they can choose to attend a class instead of working a shift on the ambulance or, alternatively, they can choose to attend on their day off and receive overtime remuneration. In comparison, SDL activities are expected to take place during downtime or time off. The authors propose that, to ensure any GOSDL endeavour is successful, arrangements should be made to allocate GOSDL time instead of an ambulance shift, or to offer remuneration if undertaken in addition to the normal shift pattern.
Recommendations for policy and practice
Recently, the authors have seen an international drive to move away from the STEMI criteria and towards the occlusion myocardial infarction (OMI) criteria for catheter lab activation (Widimský et al, 2013; Meyers and Smith, 2019), which is reflected by changes in the European Society of Cardiology (ESC) guidelines (Roffi et al, 2016; Ibanez et al, 2018).
These changes have not yet been implemented in the policy for prehospital PPCI laboratory activation in Ireland (O'Donnell, 2012). This may present a timely opportunity to implement a new ECG learning strategy within NAS.
Feasibility studies investigating the acceptability and practicality of the training interventions suggested are warranted. The interventions' effectiveness should also be investigated.
Limitations
The authors acknowledge several limitations to this research. First, one of the research authorisation conditions was to limit the sampled population to the Dublin and North Leinster regions, thus excluding approximately two-thirds of the paramedics and advanced paramedics in Ireland. Second, voluntary research often suffers from non-response bias. The primary researcher decided to incentivise participation. While this ensured a reasonable response rate, it did not eliminate the likelihood of bias. Third, the study was conducted in one jurisdiction only so the findings may not be applicable to other countries. Finally, the research took place during the COVID-19 outbreak, which rendered in-person interviews inappropriate, potentially influencing some of the results.
Conclusion
The study identified major themes appearing in the interviews of paramedics and advanced paramedics, including their lifelong learning requirements, vulnerabilities, and some expressed barriers to education. The authors proposed resources that would potentially advance ECG interpretation skills, thus possibly resulting in improved patient care.
In particular, the study identified hypothetically beneficial pre-action, in-action, and post-action learning opportunities, in the form of additional lectures online and in person, a field guide, and the implementation of an official ECG feedback mechanism.
A GOSDL programme could offer practitioners access to accredited learning resources to address gaps in knowledge that they themselves have identified. The onus would be on the employer to ensure the programme's success by allocating time or remuneration as appropriate.

